Pediatric Cardiology Fellowship Training Program
Program at a glance
- Six (6) first-year clinical fellowship positions (one (1) additional slot may be open for ROTC/military-sponsored applicants on a case-by-case basis, please contact program director)
- ACGME-accredited
- Advanced training possible in noninvasive, cath, electrophysiology, adult congenital heart disease, heart failure-transplant, pulmonary hypertension, path and research
- 66 patient beds (36 in CICU, 30 in CCU)
- 24,000 outpatient visits, 2,400 admissions, 1,000 surgeries, 1,200 catheterizations, 28,000 echocardiograms, 2,900 fetal echocardiograms per year
- State-of-the-art operating room facilities and groundbreaking fetal diagnosis and treatment center, including the Garbose Family Special Delivery Unit
- 50+ core program faculty in every major cardiac subspecialty
- Strong faculty mentoring program
- Comprehensive didactic conference schedule and professional development opportunities
- Nightfloat coverage system and limited weekend calls (reduced by clinical year) to promote work/life balance, ACGME-mandated duty hours compliance

(Left to Right) Christopher Janson, MD, (Associate Fellowship Program Director) Scott Weinreb, MD, Rebecca Josowitz, MD, Jacqueline Morrison, MD, Jeremiah Joyce, MD, Jill Hsia, MD, Lindsay Rogers, MD, (Fellowship Program Director)
Program Leadership
Program Director
Lindsay Rogers, MD, MSEd
Associate Professor of Clinical Pediatrics
Associate Program Directors
Christopher Janson, MD
Assistant Professor of Pediatrics
Laura Mercer-Rosa, MD
Associate Professor of Pediatrics
Senior Academic Affairs Coordinator
Celena Green
Clinical Competency Committee (CCC)
Chair
Lindsay Rogers, MD — Echocardiography, Cardiac Care Unit
Faculty members and areas of supervision/expertise
Jodi Chen, MD — Cardiac Critical Care
Meryl Cohen, MD — Echocardiography, Cardiac Care Unit (CCU)
Michael O’Bryne — Interventional Cardiology
David Goldberg, MD — Echocardiography, Single Ventricle Program, Outpatient
Christopher Janson, MD — Electrophysiology
Matthew O'Connor — Heart Failure/Transplant
Chitra Ravishankar, MD — Cardiac Care Unit
Susan Schachtner, MD — Cardiac Care Unit, Outpatient
Program Evaluation Committee (PEC)
Chair
Chitra Ravishankar, MD — Heart Failure
Faculty Representatives
Alexander Davidson, MD — Pulmonary Hypertension
Therese Giglia, MD — Cardiac Anticoagulation and Thrombosis
Laura Mercer-Rosa, MD — Cardiology
Shobha Natarajan, MD — Hypertension
Matthew O’Connor, MD — Heart Failure/Transplant
Felina Mille, MD — Cardiac Critical Care
Maribeth Teresczuk, MD
Grace Lee, MD
Fellow Representatives
Marc Delaney, MD
Ivor Asztalos, MD
Program overview
The pediatric cardiology fellowship at Children’s Hospital of Philadelphia is one of the nation’s oldest, largest and most well-established pediatric subspecialty training programs, with continuous ACGME accreditation since May 8, 1965.
The goals of the program are:
- To produce well-rounded pediatric cardiologists who are competent clinicians in all subspecialty areas of practice
- To develop physician scientists whose published research and investigative activity will make significant contributions to the advancement of knowledge in the field
- To create innovators and leaders in academic medicine within the field of pediatric cardiology
“I have loved my experience as a cardiology fellow at CHOP. The program leadership and division of cardiology are very supportive of the fellows and there is an excellent balance of service and education.” - Andrea L. Jones, MD, pediatric cardiology fellow
Fellows’ clinical and academic progress is monitored via monthly rotation evaluations as well as a semi-annual review process supervised by our Clinical Competency Committee (CCC), which measures Fellows’ professional growth and achievement of pediatric subspecialty training milestones in accordance with the six (6) ACGME-defined core competency areas.
While the outcomes-based core curriculum is intentionally highly structured and rigorous, fellows take an active role in shaping their own education through formal program evaluation, annual fellowship retreat and class representative participation on the Program Evaluation Committee (PEC) and other committees. Fellows are also given the opportunity to provide informal feedback to the program director during fellows’ meetings and to other teaching faculty, including medical directors, when they are on service or available to meet. Changes to the program or its stated goals are amply discussed and reviewed prior to implementation.

Scott Weinreb, MD, Rebecca Morrison, Rebecca Josowitz MD, Celena Green, (Sr. Academic Fellowship Coordinator), Jill Hsia, MD, Jeremiah Joyce, MD, and Ivor Asztalos, MD
Mentorship
To further enhance our trainees’ opportunities for success and assist them with both navigating the transition from general to subspecialty practice and meeting their professional goals and academic requirements, each trainee is paired with a personal faculty mentor and a research faculty mentor during fellowship. Personal mentors are selected for each mentee based on “model” career paths, goals and fields of interest. Fellows meet with their mentors 6-8 times per year to discuss work/life balance, career paths, review of evaluations and any concerns during training.
Research mentors are chosen by the first-year fellows at the end of the year with the help of Laura Mercer-Rosa, MD, Associate Program Director of Research.
Additionally, program leadership is always available on an ad hoc basis for resources and support.
The history, expertise and compassion that make Children’s Hospital of Philadelphia unique are also what makes it the best place for medical trainees.
Cardiac Research
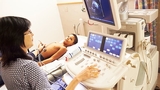
CHOP's Cardiac Center is one of the largest and most established pediatric heart programs in the world. A core part of our mission is to improve children's lives through research. With the top clinical experts in the field, our research aims to improve the health, wellbeing, and lives of all children with heart disease. Learn more about Cardiac Center research. View highlighted recent publications from the Cardiac Center.
Training Sequence
Year One
After a month-long orientation program run by the more senior fellows, the first year of the program is 90 percent clinical in focus including:
- Inpatient service
- ICU
- Echocardiography
- Cardiac catheterization
- Pathology
Night float time is also included. A weekly continuity clinic is also included.
Year Two
The second year of fellowship incorporates additional time on the non-invasive ICU and cardiac catheterization services along with EP and heart failure/transplant rotations. Additional exposure is given in the following subspecialty areas:
- Adult congenital heart disease
- Cardiac magnetic resonance imaging
- Exercise physiology
- Heart failure/transplant
- Pulmonary hypertension
In addition, five-six total months of research time is included in this year.
Year Three
In the third year of fellowship, trainees will complete the formal research block (and the required scholarly work product for professional board exam eligibility) and resume clinical work in the CICU and various cardiology clinical laboratories. They will participate in the consult service, and in some cases, will participate on the CCU in a “pretending” role.
“Senior” fellows are expected to assume a greater degree of responsibility on these rotations, often taking on certain teaching responsibilities to junior fellows and residents that are commensurate with their experience, as determined and supervised by attending faculty.
With a similar focus in mind, fellows are responsible for attending their weekly half-day continuity clinics throughout their three years of training with the exception of blocks of CCU, CICU, night float and vacation. In this manner, fellows learn effective time management from balancing patient care responsibilities with other aspects of their academic and clinical workload.
Rotations
Adult Congenital Heart Disease (ACHD)
Medical Director — Yuli Kim, MD
Faculty — Sara Partington, MD, Emily Ruckdeschel, MD
The Philadelphia Adult Congenital Heart Center is a joint venture between CHOP and the Hospital of the University of Pennsylvania. During the ACHD rotation, the fellow will gain the knowledge, skills and attitudes necessary to provide appropriate, effective and compassionate care to adults with congenital heart disease. Fellows are required to learn and review methods for taking an adult cardiac history and physical examination, and to competently make informed diagnostic and therapeutic decisions based on patient information, current scientific evidence and clinical judgment. They should be able to provide effective counseling with regard to medical issues such as pregnancy and contraception. Fellows should be aware of the unique psychosocial needs that must be met for these patients in transitioning from pediatric to adult care and participate in care coordination that reflects understanding of the capacity and limitations of the healthcare system relevant to their clinical specialty.
Cardiac Care Unit (CCU)
Medical Director — Susan Schachtner, MD
Assistant Director — Faculty — Meryl Cohen, MD, Christine Falkensammer, MD, Therese Giglia, MD, Katharine Levinson, MD, Shobha Natarajan, MD, Tamar Preminger, MD, Matthew O’Connor, MD, Chitra Ravishankar, MD, Lindsay Rogers, MD, Anita Szwast, MD
The Cardiac Care Unit (CCU) rotation is designed for the fellow to develop expertise in the acute and chronic medical management of infants and children diagnosed with congenital and acquired heart disease.
Fellows participate in daily morning rounds with the pediatric residents and cardiology attending, reviewing physical findings, laboratory results and management plans for each patient. The fellow supervises the management of medical inpatients on the service (admissions and discharges) and teaches basic cardiology topics and focused histories to the residents.
Cardiac Intensive Care Unit (CICU)
Medical Director — Venkat Shanker, MBBS
Faculty — Geoffrey Bird, MD, Joshua Blinder, MD, Marissa Brunetti, MD, Jodi Chen, MD, Andrew Costarino, MD, Aaron DeWitt, MD, Monique Gardner, MD, Michael Goldsmith, MD, David Hehir, MD, Benjamin Kozyak, MD, Felina Mille, MD, Maryam Naim, MD, Joseph Rossano, MD, Amy Romer, MD
Critically ill medical and surgical patients with cardiovascular disease are cared for in the Cardiac Intensive Care Unit (CICU) by a dedicated team of cardiologists and critical care specialists. During this rotation fellows become familiar with all aspects of care for critically ill cardiac patients including:
- Airway management and mechanical ventilation
- Preoperative stabilization
- Cardiopulmonary bypass and its sequelae
- Technical aspects of cardiac surgery and postoperative management
- Mechanical support including ECMO and VAD
Cardiology fellows work closely with critical care, cardiac anesthesia and cardiac surgery fellows in the management of all patients in the CICU, including pre- and post-operative care and participation in invasive procedures. Responsibilities include:
- Participation in morning and evening rounds with the CICU team
- Participation in night call coverage
- Preparation of weekly pre-surgical conference and monthly CICU mortality and morbidity conference
- Coordination of all appropriate pre- and post-operative testing (e.g., electrocardiograms, 24-hour ambulatory monitoring, echocardiograms and cardiac catheterization
Consult Service
Medical Director — Chitra Ravishankar, MD
Faculty — Julie Brothers, MD, Aaron Dorfman, MD, Christine Falkensammer, MD, Matthew Harris, MD, Alexa Hogarty, MD, Robert Palermo, DO, Paul Stephens, MD, Kevin Whitehead, MD
The goal of the consult service rotation, undertaken in the fellow’s second and/or third year, is to ensure that the fellow fully develops the knowledge, skills and attitudes required to provide cardiology consultation service in the evaluation and treatment of infants, children, adolescents and adults with acquired and congenital cardiac disease.
The tasks of appropriately utilizing information technology to optimize patient care, providing sensitive counseling to families, and collaborating with other members of the allied health team to refer patients from other units and specialty disciplines for further cardiac screening create a focus on practice-based learning.
Electrophysiology
Medical Director — Maully Shah, MD
Faculty — Ramesh Iyer, MD, Christopher Janson, MD, Victoria Vetter, MD

Approximately 200 procedures are performed annually in the Cardiac Electrophysiology Laboratory. Fellows rotate through this lab twice during their second or third year, learning how to use electrophysiologic information and technology to diagnose and treat various types of cardiac arrhythmia. Fellows gain experience with:
- Electrocardiographic interpretation of complex arrhythmias on standard electrocardiograms
- 24-hour ambulatory (Holter) monitors
- Transtelephonic monitors
- Acute and chronic management of arrhythmia patients
Trainees participate in daily arrhythmia rounds, all outpatient arrhythmia visits, pacemaker clinic, EP consult service, intracardiac electrophysiology studies and operative and catheter ablation procedures.
Interventional Cardiology (Cardiac Catheterization)
Medical Director — Matthew Gillespie, MD
Faculty — Yoav Dori, MD, Matthew Gillespie, MD, Michael O'Byrne, MD, Jonathan Rome, MD, Christopher Smith, MD
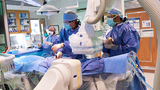
Approximately 1,400 diagnostic and therapeutic procedures are performed each year in the Cardiac Catheterization Laboratory.
Fellows participate in daily pre-catheterization conferences, present and discuss data at weekly post-catheterization conferences, and attend weekly angiogram review sessions.
By completion of fellowship, trainees are able to plan, perform and interpret a complete diagnostic study. For those with special interest in invasive cardiology, there is opportunity to develop skills in therapeutic catheterization during the latter portion of fellowship training.
Non-Invasive Imaging
Echocardiography
Medical Director — Michael Quartermain, MD
Faculty — Anirban Banerjee, MD, Meryl S. Cohen, MD, Karl Degenhardt, MD, PhD, Aaron Dorfman, MD, Christine Falkensammer, MD, Mark Fogel, MD, David Goldberg, MD, Betsy Goldmuntz, MD, Alexa Hogarty, MD, Matthew Jolley, MD, Laura Mercer-Rosa, MD, Sumekala Nadaraj, MD, Shobha Natarajan, MD, Matthew O’Connor, MD, Jack Rychik, MD, Jill Savla, MD, Amanda Shillingford, MD, Paul Stephens, MD, Anita Szwast, MD, Carol Wittlieb-Weber, MD
During the echocardiography laboratory rotation, fellows acquire the knowledge and skills necessary to correctly perform and interpret transthoracic (TTE), transesophageal (TEE) and fetal echocardiograms.
Fellows will learn to differentiate various technical modalities including M-mode, 2D, Doppler and color flow imaging, conduct proper probe selection, and to correctly identify and describe the function of the echo machine knobs. They will be able to identify the indications for various types of studies and work collaboratively with laboratory staff to build efficiency, improve communications, create quality improvement initiatives and enhance procedural and process workflow.
A weekly didactic echocardiography laboratory conference and three teaching sessions a week conducted by faculty and the senior noninvasive imaging fellow(s) provide multiple opportunities for trainees to develop and enhance their technical skills and fund of knowledge. Advanced imaging modalities are also introduced including 3D imaging and deformation imaging.
Fetal echocardiography is covered starting in second year. In addition to the busy clinical referring center, there is a weekly fetal review. Indications for fetal echocardiography, counseling of families and plan of delivery are covered during the rotation.
Exercise Physiology
Medical Director — Julie Brothers, MD,
Faculty — Julie Brothers, MD, Jonathan B. Edelson, MD, Matthew Elias, MD, Emmanuelle Favilla, MD, Alexa Hogarty, MD, Paul Stephens, MD

Fellows will learn to competently monitor patients and collect, record and interpret data from exercise studies during their rotation in the Exercise Lab. At completion of the rotation, the fellow should be able to describe the indication and protocols of a regular exercise and pharmacologic stress test, describe the equipment used, and develop a preliminary or independent interpretation of the study data depending upon the year of training (second and third year, respectively).
Magnetic Resonance Imaging
Medical Director — Mark A. Fogel, MD
Faculty — Matthew A. Harris, MD, Sara Partington, MD, Kevin Whitehead, MD
In the Cardiomagnetic Resonance Imaging Laboratory, fellows are required to observe at least 40 percent of the MRI studies conducted during the rotation. Fellows will:
- Learn to compare and contrast different types of MRIs (e.g. spin echo, cine, magnetic tagging) and be able to list the advantages and limitations of cardiac magnetic resonance as a diagnostic modality.
- Be able to correctly identify cardiac anatomy, interpret cardiac physiology and correctly synthesize diagnoses obtained from magnetic resonance studies. The fellow will be able to concisely and accurately convey pertinent data obtained from MRI at surgical conference.
Heart Failure/Transplant
Medical Director — Matthew O’Connor, MD
Faculty — Danielle Burstein, MD, Jonathan Edelson, MD, Kimberly Lin, MD, Joseph Rossano, MD, Carol Wittlieb-Weber, MD
The goal of the Cardiomyopathy/Heart Failure/Transplant rotation is that at the end of the fellowship, the fellow has the required knowledge, skills and attitudes to effectively evaluate and initiate management of infants, children and adolescents with cardiomyopathy and heart failure, and patients who have undergone cardiac transplantation.
Outpatient Clinic
Medical Director — Vivek Allada, MD
Faculty — Anirban Banerjee, MD, Meryl Cohen, MD, David J. Goldberg, MD, Shobha Natarajan, MD, Stephen Paridon, MD, Susan Schachtner, MD, Paul Stephens, MD, Anita Szwast, MD
Each of our 18 categorical first- through third-year fellows is assigned to a half-day Fellows’ outpatient clinic held on a Tuesday, Wednesday or Thursday. These clinics are staffed by two (2) attendings. The rationale is to create a “continuity of care” model wherein the fellow can see a wide range of patient referrals.
We encourage fellows to follow patients with acquired and congenital heart disease throughout their course of treatment — from inpatient unit, emergency department or primary caregiver referral to diagnosis and subsequent medical and/or surgical intervention and post-operative care.
Fellows will learn to perform a thorough cardiac-focused history and physical examination. They will learn to make informed diagnostic and therapeutic decisions, professionally counsel patients and families with cultural competence, awareness and sensitivity, and use information technology competently and efficiently to optimize patient care.
Pathology
Medical Director — Lindsay Rogers, MD
Faculty — Meryl Cohen, MD, Lindsay Rogers, MD, Jill Savla, MD
The ability of the cardiologist to provide precise anatomic diagnosis is essential to effective treatment including surgical intervention for the most complex congenital defects. During the one-month cardiac pathology rotation unique to our training program, the fellow will:
- Learn the segmental approach to cardiac diagnosis and the morphologic method of cardiac description and become acquainted with a wide variety of congenital heart defects.
- Perform a detailed examination of at least 30 postmortem specimens in the cardiac registry and review during independent study sessions with the director.
Pulmonary Hypertension
Medical Director — Alexander Davidson, MD
Faculty — Catherine Avitabile, MD, David Frank, MD, PhD, Therese Giglia, MD, Jennifer Tingo, MD
The Pulmonary Hypertension (PH) Program provides care to children with a wide variety of diagnoses that involve pulmonary vascular pathophysiology. Fellows participating in the care of our patients have the opportunity to learn about the physiology of the failing cardiovascular and pulmonary vascular systems, hemodynamic evaluation, and medical management particular to the care of patients with end-stage heart and/or lung disease. This includes those children with idiopathic PH, congenital heart disease with associated pulmonary vascular disease, cardiomyopathy with severe restrictive physiology, pulmonary vein stenosis/occlusion and right heart failure from PH associated with chronic lung disease.
Research Opportunities and Goals
Research Overview

Our fellowship program’s research curriculum has a clearly outlined sequence of goals and objectives to ensure that each fellow meets the minimum requirements for scholarly activity and a scholarly work product per the American Board of Pediatrics criteria but may also consider and incorporate graduate and post-graduate scholarship and funding opportunities for advanced specialization as part of training at CHOP.
Fellows are encouraged to begin thinking prospectively about their research work in cardiology as early as the fellowship interview/program selection.

First Year
Fellows will receive a review of the research curriculum and expectations in the fall of their first year and work with their clinical faculty mentor to identify a research faculty mentor by the end of the first year. HERE

Second Year
In the second year, fellows work with the research director and coordinator (with input from their clinical mentor and research mentor) to form a Scholarship Oversight Committee (SOC).
The entire committee will meet with the fellow and research mentor two to three times in the second and third year of training to ensure project feasibility, timeliness and efforts toward completion. The SOC will review the fellow’s individual development plan, proposed project summary (aka “white paper”) and IRB submission protocols.
In addition to meeting with the SOC, fellows have an opportunity at least once per year in the second and third year to present research to division faculty and peers at Fellows’ Research Conference. Fellows are encouraged to submit posters and abstracts to major cardiology conferences.

Third Year
The third and final year of training includes five to six months of largely uninterrupted research time, focused on project completion. Examples of scholarly activity work products per the American Board of Pediatrics may include:
- A first author or co-authored paper published in a peer-reviewed journal
- An in-depth manuscript describing a completed project
- A thesis or dissertation written in connection with pursuit of an advanced degree
- An extramural grant application that has been accepted or favorably reviewed
- A progress report for a project of exceptional complexity (e.g. a multi-year or multi-facility clinical trial)
Additional Opportunities
In the fall of the second year, depending on personal academic and career goals, the fellow may wish to consider applying for the Master of Science in Clinical Epidemiology (MSCE) or Master of Science in Translational Research programs offered by the University of Pennsylvania and/or the Division-sponsored NIH T32 funding grant.
Annual Report
Download the Cardiac Center's Annual Report for January to December 2024.
Weekly Conferences
Monday
9 a.m. — Echocardiography Teaching and Review Session
4:00 p.m. — Rotating Conference: Pediatric Cardiology Research Lecture (PCRL)
First and third Monday
7:30 a.m. — Clinical Case Conference
Second and fourth Monday
7:30 a.m. — Adult Congenital Heart Disease Conference
Second Monday — Radiology Conference Room, Level G, Perelman Center
Fourth Monday — Eighth Floor Main Conference Room
Every other month (six times per year)
7:30 a.m. — Cardiac Center Morbidity and Mortality Conference
Stokes Auditorium, First Floor Main
Tuesday
Weekly
7:30 a.m. — CT Surgery Lectures
3 p.m. — Cardiac Thrombosis Rounds
Large CICU Conference Room
First and third Tuesday
5 p.m. — MRI Conference
Radiology Conference Room, Third Floor Main
Wednesday
Weekly
7:30 a.m. — Professor Rounds
CICU, Sixth Floor Main
9 a.m. — Echocardiography Teaching and Review Session
Echo Lab Conference Room, Third Floor, Main
Noon — ECG/Holter Reading Conference
Fellows Room, Eighth Floor, 8NW25 (confirm weekly with Cardiology Fellows)
4 p.m. — Fetal Heart Conference
Fetal Conference Room, Sixth Floor Main
Thursday
Weekly
1 p.m. — Pathology Dissection Conference
4:30 p.m. — Pathology Conference
Second and fourth Thursday
7:30 a.m. — Fellows’ Teaching Conference
Monthly
7:30 a.m. — Fellows’ Research Conference
Eighth Floor Conference Room, 8NW27
Friday
Weekly
7:30 a.m. — Post-catheterization Conference
Cath/Angio Rm 6NE92, Sixth Floor Main
9 a.m. — Echocardiography Teaching and Review Session
Echo Lab Conference Room, Third Floor, Main
Noon — CICU Friday Conference
Rotating:
Week 1 – Case Conference
Week 2 – Respiratory Failure
Week 3 – Journal Club
Week 4 – Research
Annual and multi-year meetings (specialty-specific)

Fellows are encouraged to attend annual professional meetings to meet and learn from expert faculty in the field and to network with alumni and peers:
- February — Cardiology Update (“CHOP Conference”)
- March — American College of Cardiology (ACC)
- April — International Society for Heart & Lung Transplantation (ISHLT)
- May:
- June — American Society for Echocardiography (ASE)
- November — American Heart Association (AHA)
- December — Pediatric Cardiac Intensive Care Society (PCICS)
CHOP's Annual Cardiology Conference
How to Apply
Eligibility
To be eligible to apply for the Fellowship in Pediatric Cardiology, physicians:
- Must be a graduate of a U.S. or Canadian medical school or possess an ECFMG certificate and eligible J1 or H1B visa status.
- Must have completed pediatric residency training in an ACGME-accredited program.
- Must be eligible for board certification in pediatrics by the American Board of Pediatrics.
Application Requirements
Pediatric Cardiology (three-year program)
All applications for standard three (3)-year categorical fellowships must be electronically through the Electronic Residency Application Service (ERAS), the online application service of the American Association of Medical Colleges (AAMC). The annual official deadline for a completed application is August 15. If selected to interview, we try to accommodate interview date requests.
The following documents must be received by ERAS prior to consideration of your application:
- ERAS application form
- Curriculum vitae
- Personal statement
- Medical school transcript
- USMLE score reports
- Successful applicants must complete Steps 1, 2 and 3 prior to starting fellowship due to Pennsylvania licensure requirements
- Three (3) letters of recommendation (LORs)
- Educational Commission for Foreign Medical Graduates (ECFMG) certificate and visa information, if applicable
Our program participates in the National Residency Matching Program (NRMP) Pediatric Subspecialties Spring Match. Anticipated application and recruitment timeline (and notable deadlines) for the upcoming season are can be found on their site.
Senior/Advanced Fellowships
Fourth- and fifth-year fellowships (PGY-7 and PGY-8) are offered contingent on funding and availability.
In recent years, the noninvasive imaging (echo and MRI), interventional cardiology, electrophysiology and cardiac critical care practice groups have recruited trainees on a regular basis. There are also opportunities to pursue advanced training in adult congenital heart disease, heart failure/transplant, cardiac pathology, pulmonary hypertension, exercise physiology and research.
Training eligibility varies by subspecialty, though most applicants commonly will have completed a three-year fellowship in pediatric cardiology and/or pediatric critical care medicine. It is recommended that prospective advanced trainees contact the section director(s) with specific questions and concerns.
Application materials for advanced subspecialty fellowships are sent directly to the program, not through ERAS. Once completed, these files are sent to the director(s) for review. A completed fourth- and fifth-year training application will include:
- CHOP Common Graduate Medical Education Training Application (Rev. 08-2019).doc(7 pp) AND
- 4th Year HF/Transplant- Please contact Dr. Carol Wittlieb-Weber prior to application submission to confirm availability for the upcoming year.
- 4th Yr Advanced-pediatric-cardiology-subspecialty-fellowship application.pdf
- 4th Yr Advanced-pediatric-cardiology-subspecialty-fellowship application.pdf (for all subspecialties except CICU) OR
- 4th Yr Advanced-pediatric-cardiology-subspecialty-fellowship application.pdf (1 pp)
- ECHO advanced-imaging-fellowship-application-requirements.pdf
- Each Subspecialty above require the following supporting documents below, except for ERAS Form:
- CV
- Personal Statement
- (3) Letters of Recommendation
Please send materials directly to the subspecialty listed above via each email listed. Should you have submission issues, email cfp@chop.edu for any questions.
Equal Opportunity
Children’s Hospital of Philadelphia is an equal opportunity employer, committed to creating an environment where all people feel valued and respected and can contribute to their fullest potential. A non-discrimination and harassment policy is strictly enforced. No applicant for employment shall be subjected to discrimination because of race, color, sex, national origin, religion, disability, age, sexual orientation, or family status.
Other Requirements
To carry out its mission, it is of critical importance for the Children’s Hospital of Philadelphia (CHOP) to keep our patients, families and workforce safe and healthy and to support the health of our global community. In keeping with this, CHOP has mandated all workforce members (including trainees) on site at any CHOP location for any portion of their time be vaccinated for COVID-19 as a condition of employment.
This mandate also applies to workforce members or trainees performing work for CHOP at non-CHOP locations. Additionally, all workforce members based in or regularly scheduled to work at any New Jersey location are mandated to be both vaccinated and boosted for COVID-19, with booster timing consistent with applicable guidelines. The CHOP COVID-19 vaccine mandate is in alignment with applicable local, state and federal mandates. CHOP also requires all workforce members and trainees who work in patient care buildings or who provide patient care to receive an annual influenza vaccine. Employees may request exemption consideration for CHOP vaccine requirements for valid religious and medical reasons. Please note start dates may be delayed until candidates are fully immunized or valid exemption requests are reviewed. In addition, candidates other than those in positions with regularly scheduled hours in New Jersey, must attest to not using tobacco products.
Children's Hospital of Philadelphia is an equal opportunity employer. We do not discriminate on the basis of race, color, gender, gender identity, sexual orientation, age, religion, national or ethnic origin, disability, protected veteran status or any other protected category. CHOP is a VEVRAA Federal Contractor seeking priority referrals for protected veterans.
CHOP is committed to building an inclusive culture where employees feel a sense of belonging, connection, and community within their workplace. We are a team dedicated to fostering an environment that allows for all to be their authentic selves. We are focused on attracting, cultivating, and retaining diverse talent who can help us deliver on our mission to be a world leader in the advancement of healthcare for children.
We strongly encourage all candidates of diverse backgrounds and lived experiences to apply.
For More Information
If you are interested in fellowships at the Cardiac Center, please contact the individuals listed below.
Pediatric Cardiology (Core Program):
Contact Lindsay Rogers, MD, Program Director, at 215-590-6379 or rogersl1@chop.edu.
Adult Congenital Heart Disease
Contact Yuli Kim, MD, Program Director, at 215-615-3388 or KimY@chop.edu.
Cardiac Critical Care
Contact Jodi Chen, MD, Program Director, at 215-590-2367 or chenjo@chop.edu. (Learn more about the Pediatric Cardiac Critical Care Fellowship)
Electrophysiology
Contact Maully Shah, MBBS, Program Director, at 215-590-2230 or shahm@chop.edu.
Heart Failure – Heart Transplant
Contact Carol Wittlieb Weber, MD, Program Director, at 267-426-2882 or wittliebc@chop.edu.
Interventional Cardiology (Cardiac Catheterization)
Contact Matthew Gillespie, Program Director, at 215-590-1790 or gillespie@chop.edu.
Non-Invasive Imaging (Pediatric Echocardiography)
Contact Laura Mercer-Rosa, MD, Associate Program Director, at 215-590-3274 or mercerrosal@chop.edu.
Non-Invasive Imaging – (Pediatric Magnetic Resonance Imaging)
Contact Mark A. Fogel, MD, Program Director, at 215-590-3354 or fogel@chop.edu, or Matthew A. Harris, MD, Associate Program Director, at 215-590-3354 or harrismat@chop.edu.
Current Fellows
First Year
Samuel N. DeSantis, M.D.
Medical School: New York Medical College
Residency: New York Presbyterian, Columbia Irving University Medical Center, General Pediatrics
Jake Faultersack, MD
Medical School: University of Wisconsin School of Medicine and Public Health
Residency: University of North Carolina, General Pediatrics
Nathan Markiewitz MD, MA
Graduate Degree: University of North Carolina at Chapel Hill, Quantitative Psychology
Medical School: Perelman School of Medicine at the University of Pennsylvania
Residency: Children's Hospital of Philadelphia, General Pediatrics
Harper Robinson, MD
Medical School: NYU Long Island School of Medicine
Residency: Johns Hopkins Harriet Lane Residency, General Pediatrics
Kaushik Parvathaneni, MD
Medical School: Johns Hopkins University
Residency: Stanford University, Pediatrics
Amy Scheel, MD, MPH
Medical School: Emory University School of Medicine
Residency: Children's Hospital of Philadelphia, General Pediatrics
Shelby Scola, MD
Medical School: Boston University School of Medicine
Residency: Children's Hospital of Philadelphia, General Pediatrics
Second Year
Medical School: Lake Erie College of Osteopathic Medicine
Residency: Levine Children's Hospital, General Pediatrics
Medical School: Medical University of South Carolina College of Medicine
Residency: Boston Combined Residency Program Boston Children's Hospital/ Boston Medical Center, General Pediatrics
Fellowship: Children's Hospital of Philadelphia, Pediatric Critical Care
Medical School: Renaissance School of Medicine at Stony Brook University
Residency: Children's Hospital of Philadelphia, General Pediatrics
Medical School: Dr. D.Y. Patil Pratishthans Medical College
Residency: Children's Hospital of Philadelphia, Combined General Pediatrics/Genetics
Medical School: Johns Hopkins University School of Medicine
Residency: University of California San Francisco School of Medicine, General Pediatrics
Medical School: Case Western Reserve University School of Medicine
Residency: Children’s Hospital of Philadelphia, General Pediatrics
Medical School: Case Western Reserve University School of Medicine
Residency: Children’s Hospital of Philadelphia, General Pediatrics
Third Year
Medical School: Case Western Reserve University School of Medicine
Residency: Boston Combined Residency Program Boston Children's Hospital, General Pediatrics
Medical School: University of Maryland School of Medicine
Residency: Duke University Hospital Program, Internal Medicine & General Pediatrics
Medical School: Aga Khan University Medical College
Residency: Cleveland Clinic Children's, General Pediatrics
Medical School: Cleveland Clinic Lerner College of Medicine of Case Western Reserve University
Residency: Children’s Hospital of Philadelphia, General Pediatrics
Medical School: University of Michigan Medical School
Residency: Children’s Hospital of Philadelphia, General Pediatrics
Medical School: Loyola University Chicago Stritch School of Medicine
Residency: Ohio State University, Nationwide Children’s Hospital, Internal Medicine & General Pediatrics







